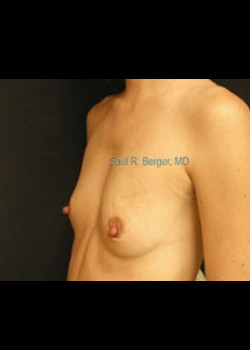
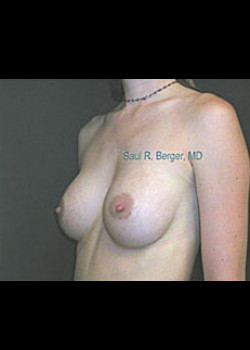
Case Details
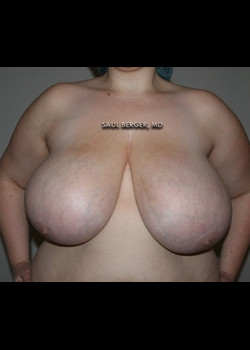
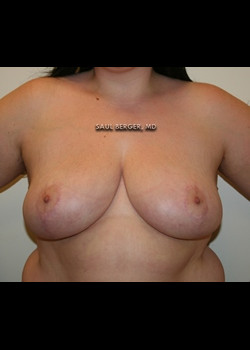
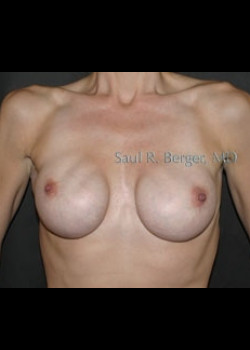
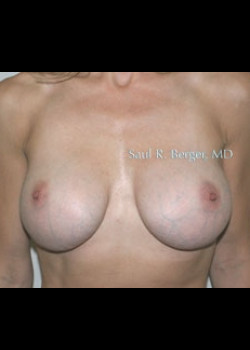
Breast Reconstruction with TRAM Flap after mastectomy (no implants used).
View Angle: front


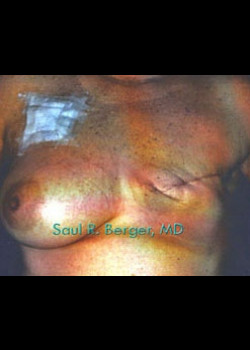
Before
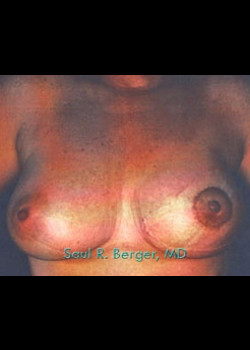
After