Rhinoplasty, or surgery to reshape the nose, is one of the most common of all plastic surgery procedures. Rhinoplasty can reduce or increase the size of your nose, change the shape of the tip or the bridge, narrow the span of the nostrils, or change the angle between your nose and your upper lip. It may also correct a birth defect or injury, or help relieve some breathing problems.
The Best Candidates For Rhinoplasty
The best candidates for rhinoplasty are people who are looking for improvement, not perfection, in the way they look. If you’re physically healthy, psychologically stable, and realistic in your expectations, you may be a good candidate.
Rhinoplasty can be performed to meet aesthetic goals or for reconstructive purposes-to correct birth defects or breathing problems.
Age may also be a consideration. Many surgeons prefer not to operate on teenagers until after they’ve completed their growth spurt-around 14 or 15 for girls, a bit later for boys. It’s important to consider teenagers’ social and emotional adjustment, too, and to make sure it’s what they, and not their parents, really want.
Planning Your Surgery
Good communication between you and your physician is essential. In your initial consultation, the surgeon will ask what you’d like your nose to look like, evaluate the structure of your nose and face, and discuss the possibilities with you. He or she will also explain the factors that can influence the procedure and the results. These factors include the structure of your nasal bones and cartilage, the shape of your face, the thickness of your skin, your age, and your expectations.
Your surgeon will also explain the techniques and anesthesia he or she will use, the type of facility where the surgery will be performed, the risks and costs involved, and any options you may have.
Be sure to tell your surgeon if you’ve had any previous nose surgery or an injury to your nose, even if it was many years ago. You should also inform your surgeon if you have any allergies or breathing difficulties; if you’re taking any medications, vitamins, or recreational drugs; and if you smoke.
The Surgery
Rhinoplasty usually takes an hour or two, though complicated procedures may take longer. During surgery the skin of the nose is separated from its supporting framework of bone and cartilage, which is then sculpted to the desired shape. The nature of the sculpting will depend on your problem and your surgeon’s preferred technique. Finally, the skin is redraped over the new framework.
When the surgery is complete, a splint will be applied to help your nose maintain its new shape. Nasal packs or soft plastic splints also may be placed in your nostrils to stabilize the septum, the dividing wall between the air passages.
All Surgery Carries Some Uncertainty And Risk
When rhinoplasty is performed by a qualified plastic surgeon, complications are infrequent and usually minor. Nevertheless, there is always a possibility of complications, including infection, nosebleed, or a reaction to the anesthesia. You can reduce your risks by closely following your surgeon’s instructions both before and after surgery.
Side Effects Of Rhinoplasty
After surgery, small burst blood vessels may appear as tiny red spots on the skin’s surface; these are usually minor but may be permanent. As for scarring, when rhinoplasty is performed from inside the nose, there is no visible scarring at all; when an “open” technique is used, or when the procedure calls for the narrowing of flared nostrils, the small scars on the base of the nose are usually not visible.
Recovery From Rhinoplasty
After surgery-particularly during the first twenty-four hours-your face will feel puffy, your nose may ache, and you may have a dull headache. You can control any discomfort with the pain medication prescribed by your surgeon. Plan on staying in bed with your head elevated for the first day.
You’ll notice that the swelling and bruising around your eyes will increase at first, reaching a peak after two or three days. Applying cold compresses will reduce this swelling and make you feel a bit better. In any case, you’ll feel a lot better than you look. Most of the swelling and bruising should disappear within two weeks or so.
If you have nasal packing, it will be removed after a few days and you’ll feel much more comfortable. By the end of one or, occasionally, two weeks, all dressings, splints, and stitches should be removed.
In the days following surgery, when your face is bruised and swollen, it’s easy to forget that you will be looking better. In fact, many patients feel depressed for a while after plastic surgery-it’s quite normal and understandable.
Rest assured that this stage will pass. Day by day, your nose will begin to look better and your spirits will improve. Within a week or two, you’ll no longer look as if you’ve just had surgery.
Still, healing is a slow and gradual process. Some subtle swelling may be present for months, especially in the tip. The final results of rhinoplasty may not be apparent for a year or more.

Before surgery, these rhinoplasty patients have large, slightly hanging noses, with a hump and an enlarged tip.
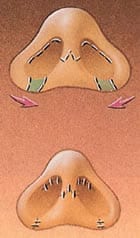
If your nostrils are too wide, the surgeon can remove small wedges of skin form their base, bringing them closer together.

Incisions are made inside the nostrils or at the base of the nose, providing access to the cartilage and bone, which can then be sculpted into shape.

The surgeon removes the hump using a chisel or a rasp, then brings the nasal bones together to form a narrower bridge. Cartilage is trimmed to reshape the tip of the nose.

Trimming the septum improves the angle between the nose and upper lip.

A splint made of tape and an overlay of plastic, metal, or plaster is applied to help the bone and cartilage of the nose maintain their new shape.

After surgery, the patient has a smaller nose, a straighter bridge, a well defined nasal tip, and an improved angle between the nose and upper lip.
Schedule Your Rhinoplasty Consult in Burbank, CA!
Contact board certified plastic surgeon Dr. Saul Berger if you wish to learn more about the Rhinoplasty procedure, or if you wish to determine whether you are a candidate for surgery. You can a schedule a consultation by calling 818.245.6101, or by filling out our online contact form. Our practice serves Burbank and the surrounding areas of California.
Content courtesy of PlasticSurgery.org